Efficacy of micronized progesterone-based preparations used to prevent placental insufficiency: an experimental study
DOI:
https://doi.org/10.18413/rrpharmacology.12.1030Аннотация
Introduction: Progestogen-based drugs have anti-ischemic, antispasmodic, and immunomodulatory effects. Therefore, studying the effect of micronized progesterone (MP) on the inflammatory process in the placenta is of great importance.
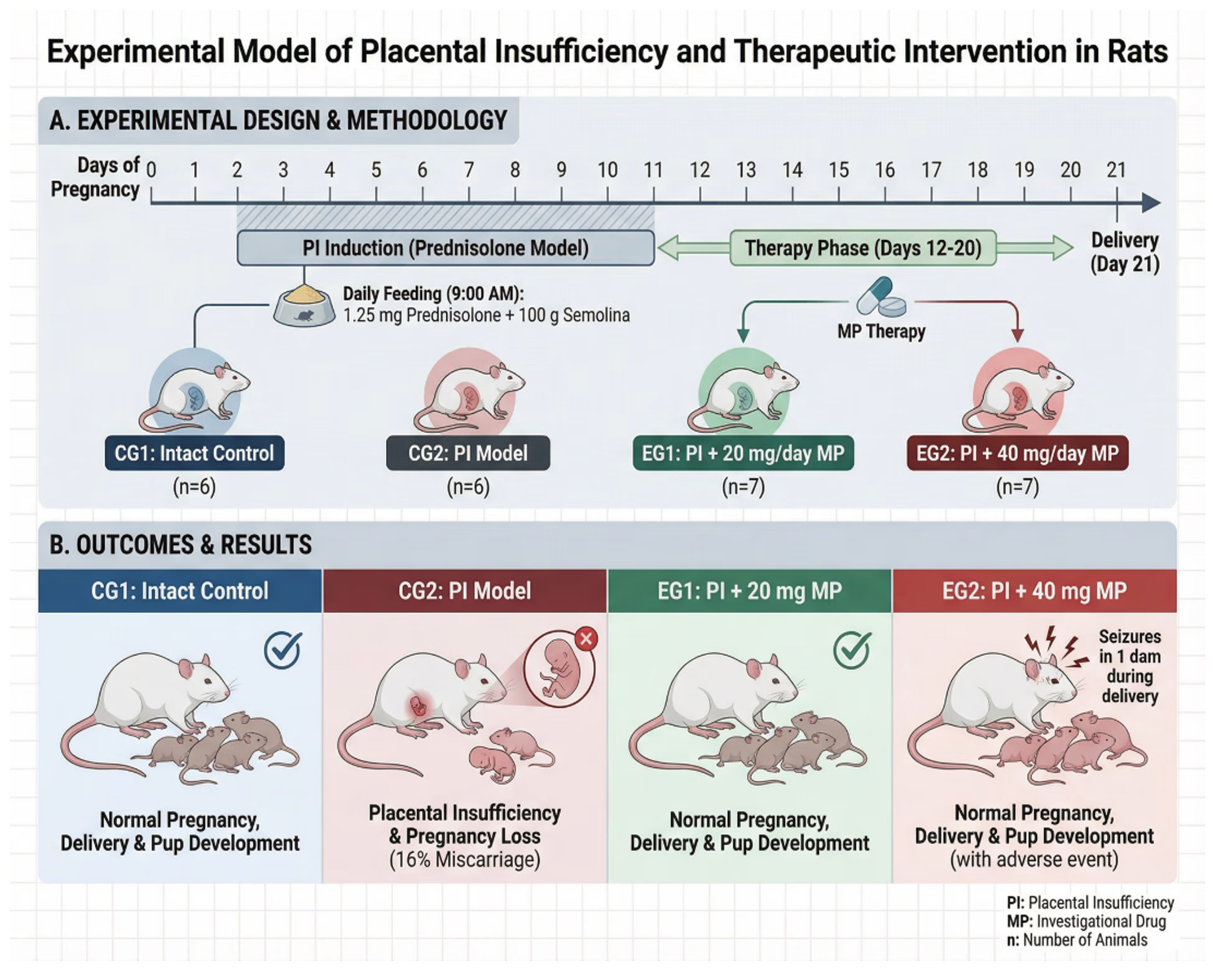
Materials and Methods: Four observation groups were formed: Control Group 1 (CG1, n=6) – intact rats; Control Group 2 (CG2, n=6) – pregnant rats with simulated placental insufficiency; Experimental Group 1 (EG1, n=7) – rats with simulated placental insufficiency that received MP dosage 20 mg/day; Experimental Group 2 (EG2, n=7) – rats with simulated placental insufficiency that received MP dosage 40 mg/day. An analysis of the placenta, anthropometric parameters of the fetuses, and physical development parameters of the offspring was conducted. Histological and immunohistochemical analyses of the placentas were performed.
Results and Discussion: Miscarriage was observed in 16% of animals from CG2, which did not receive MP therapy, compared to rats from CG1. In intact CG1 and EG1 rats, the course of pregnancy, parturition, and developmental parameters of the pups were within physiological norms. In rats from EG2, the course of pregnancy and parturition, the condition of rat pups did not differ from the physiological norm; however, one rat developed convulsions during birth. Immunohistochemical analysis revealed reduced inflammatory manifestations in the placenta of rats treated with MP, compared to animals from the control group that did not receive pharmacological correction.
Conclusion: Under experimental conditions, MP can prolong pregnancy to physiological norms and have a positive effect on the physical development of the offspring.
Графическая аннотация
Ключевые слова:
pregnancy, micronized progesterone, newborns, placental insufficiencyБиблиографические ссылки
Abourida Y, Rebahi H, Oussayeh I, Chichou H, Fakhir B, Soummani A (2020) Management of severe COVID-19 in pregnancy. Case Reports in Obstetrics and Gynecology 2020: 8852816. https://doi.org/10.1155/2020/8852816[PubMed] [РМС]
Adamyan LV, Vechorko VI, Konysheva OV, Kharchenko EI (2021) Pregnancy and COVID-19: Current issues (literature review). Russian Journal of Human Reproduction [Problemy Reproduktsii] 27(3):70–77. https://doi.org/10.17116/repro20212703170 [in Russian]
Artem'eva KA, Ponomarenko EA, Patsaev TD, Kuznetsova EV, Kondashevskaya MV, Mnikhovich MV, Deev RV, Bochkov VV, Nizyaeva NV, Demidova AS (2025) Morphofunctional characteristics of the placenta in experimental preeclampsia. Journal of Anatomy and Histopathology [ZHurnal Anatomii i Gistopatologii] 14(1): 21–28. https://doi.org/10.18499/2225-7357-2025-14-1-21-28 [in Russian]
Arzhanykh YV, Batishcheva GA, Khoroshikh NV, Khoroshikh AO (2024) Pharmacotherapy and perinatal outcomes of a new coronavirus infection according to data from Voronezh hospitals. Scientific and Medical Bulletin of the Central Black Earth Region [Nauchno-Meditsinskii Vestnik Tsentral’nogo CHernozem’ya] 2(96): 24–28. [in Russian]
Baergen RN, Heller DS (2020) Placental pathology in COVID-19 positive mothers: preliminary findings. Pediatric and Developmental Pathology 23(3):177–180. https://doi.org/10.1177/1093526620925569 [PubMed] [РМС]
Bazer FW, Wu G, Spencer TE, Johnson GA, Burghardt RC, Bayless K (2010) Novel pathways for implantation and establishment and maintenance of pregnancy in mammals. Molecular Human Reproduction 16(3):135–152. https://doi.org/10.1093/molehr/gap095 [PubMed] [РМС]
Bogdanova IM, Boltovskaya MN (2019) Functional and phenotypic characteristics of classical (M1) and alternatively activated (M2) macropfages and their role during normal and pathological pregnancy (literature review). Russian Journal of Human Reproduction [Problemy Reproduktsii] 25(5):110–118. https://doi.org/10.17116/repro201925051110 [in Russian]
Bruno DL (2003) Natural progesterone and its features. Russian Bulletin of Obstetrician – Gynecologist [Rossiiskii Vestnik Akushera-Ginekologa] 3(3):27-30. [in Russian]
Chebotareva JJ, Ovsyannikov VG, Hutieva MY (2013) Modeling of preeclampsia in the experiment in rats. Vladikavkaz Biomedical Journal [Vladikavkazskii Mediko-Biologicheskii Vestnik] 17 (26): 54–58. [in Russian]
Chebotareva JJ, Ovsyannikov VG, Hutieva MY, Podgorny IV (2017) The role of glucocorticoid dysregulation in the development of gestational pyelonephritis, placental insufficiency in the experiment. Nephrology [Nefrologiya] 21(5): 76–79. [in Russian]
Chen M, Drury JE, Penning TM (2011) Substrate specificity and inhibitor analyses of human steroid 5β-reductase (AKR1D1). Steroids 76(5):484–490. https://doi.org/10.1016/j.steroids.2011.01.003 [PubMed] [РМС]
Dall’Asta A, Melito C, Morganelli G, Lees C, Ghi T (2023) Determinants of placental insufficiency in fetal growth restriction. Ultrasound in Obstettrics and Gynecology 61(2): 152–157. https://doi.org/10.1002/uog.26111 [PubMed]
Dobrokhotova Y, Dzhokhadze LS, Kuznetsov PA, Kozlov PV (2019) Placental Insufficiency: A modern View. Moscow, 66 рр. [in Russian]
Fleming AS, Ruble D, Krieger H, Wong PY (1997) Hormonal and experiential correlates of maternal responsiveness during pregnancy and the puerperium in human mothers. Hormones and Behavior 31(2): 145–158. https://doi.org/10.1006/hbeh.1997.1376 [PubMed]
Gilbert JS, Ryan MJ, LaMarca BB, Sedeek M, Murphy SR, Granger JP (2008) Pathophysiology of hypertension during preeclampsia: linking placental ischemia with endothelial dysfunction. American Journal of Physiology 294(2): 541–550. [PubMed]
Gumusoglu SB, Chilukuri AS, Hing BQ (2021) Altered offspring neurodevelopment in an arginine vasopressin preeclampsia model. Translational Psychiatry 11(1): 79. https://doi.org/10.1038/s41398-021-01205-0 [PubMed] [РМС]
Halperin R, Peller S, Rotschild M, Bukovsky I, Schneider D (2000) Placental apoptosis in normal and abnormal pregnancies. Gynecologic and Obstetric Investigation 50(2): 84–87. https://doi.org/10.1159/000010287 [PubMed]
Ishutina NA, Andrievskaya IA (2021) Prostaglandins and their role in the early periods of embryonic development (literature review) Bulletin of Physiology and Pathology of Respiration [Byulleten' Fiziologii i Patologii Dykhaniya] (80): 129–137. https://doi.org/10.36604/1998-5029-2021-80-129-137 [in Russian]
Ivanov DO, Alexandrova EM, Harutyunyan TG (2019) Guide to perinatology. SPb.: Informnavigator 2: 936. [in Russian]
Khutieva MY (2018) Mechanisms of Formation of Gestational Complications in Pregnant Women (Clinical and Experimental Study). PhD Thesis, Peoples' Friendship University of Russia, Moscow, 85 рр. [in Russian]
Kudryavtseva EV, Martirosyan SV, Utamuradova SU (2022) Covid - 19 and placenta – associated pregnancy complications: Is there a connection? Ural Medical Journal [Ural'skii Meditsinskii ZHurnal] 21(4): 78–84. [in Russian]
Lipatov IS, Tezikov YV, Kalinkina OB, Tyutyunnik VL, Kan NE, Mayorova MO, Yakovleva MA (2022) The relationship of the new coronavirus infection with the formation of fetal growth retardation. Obstetrics and Gynecology [Akusherstvo i Ginekologiya] (2): 53–62. https://dx.doi.org/10.18565/aig.2022.260 [in Russian]
Lledo PM, Alonso M, Grubb MS (2006) Adult neurogenesis and functional plasticity in neuronal circuits. Nature Reviews. Neuroscience 7(3): 179–193. https://doi.org/10.1038/nrn1867 [PubMed]
Matsiuk YR, Baraban OV (2012) Placenta structure in rats at different stages of normal pregnancy. Journal of GrSMU [ZHurnal Grodnenskogo Gosudarstvennogo Meditsinskogo Universiteta] 1(37): 54–57. [in Russian]
Milovanov AP (2010) Morphological characteristics of the second wave of cytotrophoblastic invasion. Archive of Pathology [Arkhiv Patologii] 72(1): 3–6.[in Russian]
Milyutina YP, Shcherbitskaya AD, Saltykova ED, Kozina LS, Zhuravin IA, Nalivaeva NN, Arutyunyan AV (2017) Metabolic disorders in the placenta and brain of fetuses of pregnant rats during experimental hyperhomocysteinemia. Sechenov Russian Physiological Journal [Rossiiskii Fiziologicheskii ZHurnal im. I.M. Sechenova] 103(11): 1280–1291. [in Russian]
Minchenko DO, Tsymbal DO, Riabovol OO (2019) Hypoxic regulation of EDN1, EDNRA, EDNRB, and ECE1 gene expressions in ERN1 knockdown U87 glioma cells. Endocrine Regulations 53(4): 250–262.https://doi.org/10.2478/enr-2019-0025 [PubMed]
Niringiyumukiza JD, Cai H, Xiang W (2018) Prostaglandin E2 involvement in mammalian female fertility: ovulation, fertilization, embryo development and early implantation. Reproductive Biology and Endocrinology 16(1): 43. https://doi.org/10.1186/s12958-018-0359-5 [PubMed] [РМС]
Ovsyannikov VG, Chebotareva Y, Podgorny IV (2019) Modeling of gestational complications in an experiment on rats. Humans and Their Health [CHelovek i Ego Zdorov’e] (1): 114–123. [in Russian]
Patel FA, Clifton VL, Chwalisz K, Challis JR (1999) Steroid regulation of prostaglandin dehydrogenase activity and expression in human term placenta and chorio-decidua in relation to labor. The Journal of Clinical Endocrinology and Metabolism 84(1): 291–299. https://doi.org/10.1210/jcem.84.1.5399 [PubMed]
Petrova UL, Shmakov RG (2022) The 2019 novel coronavirus infection and pregnancy: What do we know? Obstetrics and Gynecology [Akusherstvo i Ginekologiya] (2): 4–11. [in Russian]
Rets YV (2008) The importance of fetal corticocatecholamine hormones in the pathogenesis of chronic placental insufficiency. Obstetrics and Gynecology [Akusherstvo i Ginekologiya] (1): 44–48.[in Russian]
Romero R, Stanczyk FZ (2013) Progesterone is not the same as 17α-hydroxyprogesterone caproate: Implications for obstetrical practice. American Journal of Obstetrics and Gynecology 208(6): 421–426. [PubMed] [РМС]
Ruleva AV (2007) The role of biogenic amines in the formation of placental insufficiency in gestosis. PhD Thesis, Research Institute of Obstetrics and Gynecology RAMN, Saint Petersburg, 27рр.[in Russian]
Sanaeva MD, Dudareva Yu (2022) Disease course, obstetric and perinatal outcomes in pregnant women with COVID-19 (literature review). Clinician [Lechashchii Vrach] 5(25): 20–24. [in Russian]
Vishnyakova PA, Yelchaninov AV, Kiseleva VV, Muminova KT, Khodzhaeva ZS, Eremina IZ, Fatkhutdinov TH (2022) The role of placental macrophages in physiological pregnancy and preeclampsia. Obstetrics and Gynecology [Akusherstvo i Ginekologiya] 4: 5–12. https://dx.doi.org/10.18565/aig.2022.4.5-12 [in Russian]
Volchek IА, Novozhenov VG, Gladko OV, Yakovleva LM (2025) Role of prostaglandin F2α in the pathogenesis of inflammatory processes. Bulletin of the Medical Institute of Continuing Education [Vestnik Meditsinskogo Instituta Nepreryvnogo Obrazovaniya] 5(3): 11–14. [in Russian]
Zhao Y, Xiong W, Li C (2023) Hypoxia-induced signaling in the cardiovascular system: pathogenesis and therapeutic targets. Signal Transduction and Targeted Therapy 8(1): 431. https://doi.org/10.1038/s41392-023-01652-9 [PubMed] [РМС]
Zhguleva AS, Zementova MS, Selkov SA, Sokolov DI (2024) M1/M2 macrophages: Origin, phenotype, production methods, interaction with natural killers and trophoblast. Medical Immunology [Meditsinskaya Immunologiya] 26(3): 427–428. doi:10.15789/1563-0625-MMO-2877 [in Russian]
Zolotukhina YV (2024) The impact of pharmacotherapy on the structure of placental disorders in women with SARS-COV-2 infection in the second trimester of gestation. Medical Scientific Bulletin of Central Chernozemye [Nauchno-Meditsinskii Vestnik Central’nogo Chernozem’ya] 2(25): 17–20. [in Russian]
Загрузки
Опубликован
Как цитировать
Выпуск
Раздел
Лицензия
Copyright (c) 2026 Batishcheva GA, Zolotukhina YV, Shishkina VV, Khoroshikh NV, Samoylenko TV, Zhilyaeva OD, Zolotareva SN, Ivanova EE, Khoroshikh AO

Это произведение доступно по лицензии Creative Commons «Attribution» («Атрибуция») 4.0 Всемирная.
 Русский
Русский
 English
English

