Evaluation of the neuroprotective effects of synthetic erythropoietin derivatives in a mouse model of mild and moderate hypoxic-ischemic encephalopathy
DOI:
https://doi.org/10.18413/rrpharmacology.12.1071Abstract
Introduction: Hypoxic-ischemic encephalopathy (HIE) is a leading cause of neonatal brain injury and long-term neurodevelopmental impairment, and current therapies only partially prevent adverse outcomes. Although recombinanterythropoietin is neuroprotective via EPOR–CD131 (βcR), its use is limited by hematopoietic side effects, motivating evaluation of non-hematopoietic peptide analogs such as Ara-290 and Epobis in HIE.
Materials and Methods: Neonatal hypoxia-ischemia was induced in 9-day-old CD-1 mice (n = 204) using a modified Rice–Vannucci model, and animals were stratified into mild and moderate severity groups 3 hours later by laser speckle contrast imaging (RFLSI-ZW) before assignment to treatment. EPO (5000 IU/kg) and Epobis (20 mg/kg) were administered subcutaneously every 24 hours and Ara-290 (30 µg/kg) intraperitoneally every 12 hours for 7 days, after which motor-coordination performance, macroscopic lesion volume, and expression of IL-4, IL-1b, IL-6, and TNF-α were assessed.
Results: In both mild and moderate HIE, Epobis provided the most consistent neuroprotection, improving motor performance and neurological outcomes and being the only treatment to significantly reduce macroscopic lesion volume. EPO produced moderate functional benefits, whereas Ara-290 showed a less stable efficacy profile, with limited or absent effects in several behavioral and morphological endpoints.
Conclusion: In mild HIE, Epobis showed the strongest neuroprotection, improving motor-coordination performance, reducing neurological deficits, and producing the greatest reduction in macroscopic lesion volume, whereas EPO and Ara-290 had only moderate effects. In moderate HIE, Epobis and EPO most consistently improved motor outcomes, but only Epobis significantly reduced lesion volume and neurological symptom severity and produced the most pronounced immunomodulation.
Graphical Abstract
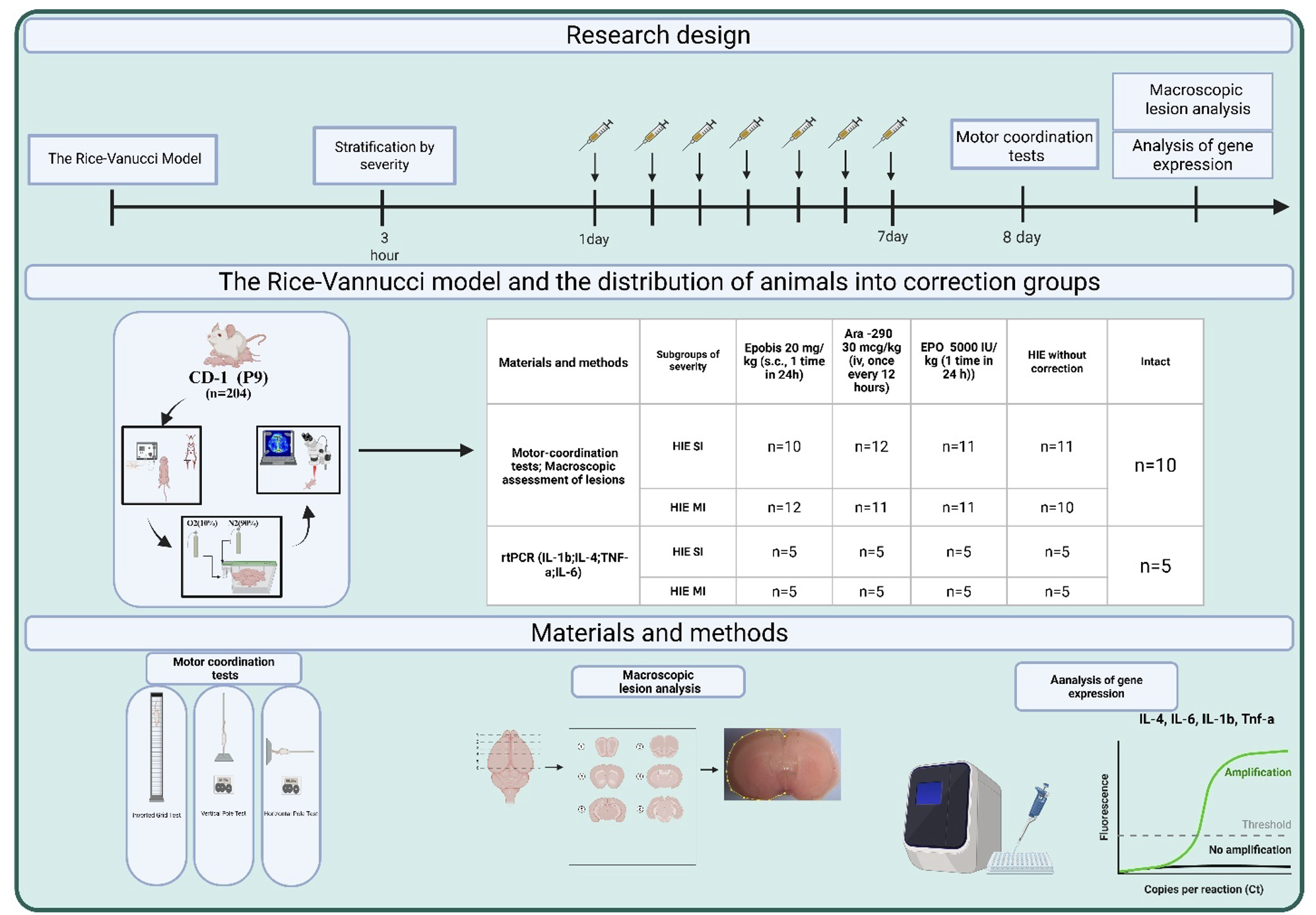
Keywords:
hypoxic-ischemic encephalopathy, motor-coordination functions, Epobis, Ara-290, erythropoietin, laser speckle contrast imagingReferences
Anusornvongchai T, Nangaku M, Jao TM, Wu CH, Ishimoto Y, Maekawa H, Tanaka T, Shimizu A, Yamamoto M, Suzuki N, Sassa R, Inagi R (2018) Palmitate deranges erythropoietin production via transcription factor ATF4 activation of unfolded protein response. Kidney International 94(3): 536–550. https://doi.org/10.1016/j.kint.2018.03.011 [PubMed]
Arnautovic T, Sinha S, Laptook AR (2024). Neonatal hypoxic-ischemic encephalopathy and hypothermia treatment. Obstetrics and Gynecology 143(1): 67–81. https://doi.org/10.1097/AOG.0000000000005392 [PubMed] [PMC]
Chakkarapani E, de Vries LS, Ferriero DM, Gunn AJ (2025) Neonatal encephalopathy and hypoxic-ischemic encephalopathy: The state of the art. Pediatric Research https://doi.org/10.1038/s41390-025-03986-2 [PubMed] [PMC]
Chan NH, Hawkins CC, Rodrigues BV,Cornet MC, Gonzalez FF, Wu YW (2025). Neuroprotection for neonatal hypoxic-ischemic encephalopathy: A review of novel therapies evaluated in clinical studies. Developmental Medicine and Child Neurology 67(5): 591–599. https://doi.org/10.1111/dmcn.16184 [PubMed] [PMC]
Collino M, Thiemermann C, Cerami A, Brines M (2015) Flipping the molecular switch for innate protection and repair of tissues: Long-lasting effects of a non-erythropoietic small peptide engineered from erythropoietin. Pharmacology and Therapeutics 151: 32–40. https://doi.org/10.1016/j.pharmthera.2015.02.005 [PubMed]
Dmytriyeva O, Pankratova S, Korshunova I, Walmod PS (2016) Epobis is a nonerythropoietic and neuroprotective agonist of the erythropoietin receptor with anti-inflammatory and memory enhancing effects. Mediators of Inflammation 2016: 1346390. https://doi.org/10.1155/2016/1346390 [PubMed] [PMC]
Dolan F, Wintermark P (2025) Updates in treatment of hypoxic-ischemic encephalopathy. Clinics in Perinatology 52(2): 321–343.https://doi.org/10.1016/j.clp.2025.02.010 [PubMed]
Fong H, Zhou B, Feng H, Luo C, Bai B, Zhang J, Wang Y (2024) Recapitulation of structure-function-regulation of blood-brain barrier under (patho)physiological conditions. Cells 13(3): 260. https://doi.org/10.3390/cells13030260 [PubMed] [PMC]
Glass HC, Wood TR, Comstock BA, Numis AL, Bonifacio SL, Cornet MC, Gonzalez FF, Morell A, Kolnik SE, Li Y, Mathur A, Mietzsch U, Wu TW, Wusthoff CJ, Thoresen M, Heagerty PJ, Juul SE, Wu YW (2024) Predictors of death or severe impairment in neonates with hypoxic-ischemic encephalopathy. JAMA Network Open 7(12): e2449188. https://doi.org/10.1001/jamanetworkopen.2024.49188[PubMed] [PMC]
Juul SE, Yachnis AT, Rojiani AM, Christensen RD (1999). Immunohistochemical localization of erythropoietin and its receptor in the developing human brain. Pediatric and Developmental Pathology 2(2): 148–158. https://doi.org/10.1007/s100249900103 [PubMed]
Konrad J, Chau V, Selvanathan T (2025) Advances in neonatal hypoxic-ischemic encephalopathy. Pediatric Clinics of North America 72(5): 939–955. https://doi.org/10.1016/j.pcl.2025.05.006 [PubMed]
Lissy M, Ode M, Roth K (2011) Comparison of the pharmacokinetic and pharmacodynamic profiles of one US-marketed and two European-marketed epoetin alfas: A randomized prospective study. Drugs in R & D 11(1): 61–75. https://doi.org/10.2165/11588270-000000000-00000 [PubMed] [PMC]
Pankratova S, Gu B, Kiryushko D, Korshunova I, Køhler LB, Rathje M, Bock E, Berezin V (2012) A new agonist of the erythropoietin receptor, Epobis, induces neurite outgrowth and promotes neuronal survival. Journal of Neurochemistry 121(6): 915–923. https://doi.org/10.1111/j.1471-4159.2012.07751.x [PubMed]
Pokrovskii V, Lapin K, Antonova V, Korokin M, Gudyrev O, Gureev V, Korokina L, Scheblykina O, Nesterov A, Maslinikova M, Chatsky I, Mukhamedov D, Pokrovskii M (2026) Use of laser speckle contrast imaging for distribution of animals by severity of brain tissue damage in a neonatal hypoxia-ischemia model in mice. Brain Sciences 16: 102. https://doi.org/10.3390/brainsci16010102 [PubMed] [PMC]
Pokrovsky VM, Chatsky IV, Maslinikova MR, Zabolotskikh NV, Nesterov AV, Popov NV, Korokin MV (2025) Investigation of behavioral characteristic changes in animals with varying injury severity following brain tissue damage in a mouse model of neonatal hypoxia-ischemia during the juvenile period. Research Results in Pharmacology 11(4): 282–292. https://doi.org/10.18413/rrpharmacology.11.863
Schneider Gasser EM, Elliot-Portal E, Arias-Reyes C, Losantos-Ramos K, Khalid K, Ogunshola O, Soliz J (2019). Developmental expression patterns of erythropoietin and its receptor in mouse brainstem respiratory regions. Respiratory Physiology and Neurobiology 267: 12–19. https://doi.org/10.1016/j.resp.2019.05.012 [PubMed]
Sheldon RA, Windsor C, Ferriero DM (2018) Strain-related differences in mouse neonatal hypoxia-ischemia. Developmental Neuroscience 40(5–6): 490–496. https://doi.org/10.1159/000495880 [PubMed] [PMC]
Simon F, Floros N, Ibing W, Schelzig H, Knapsis A (2019) Neurotherapeutic potential of erythropoietin after ischemic injury of the central nervous system. Neural Regeneration Research 14(8): 1309–1312. https://doi.org/10.4103/1673-5374.253507 [PubMed] [PMC]
Walas W, Wilińska M, Bekiesińska-Figatowska M, Halaba Z, Śmigiel R (2020). Methods for assessing the severity of perinatal asphyxia and early prognostic tools in neonates with hypoxic-ischemic encephalopathy treated with therapeutic hypothermia. Advances in Clinical and Experimental Medicine 29(8): 1011–1016. https://doi.org/10.17219/acem/124437 [PubMed]
Wang R, Wu X, Zhao H, Min L, Tao Z, Ji X, Luo Y (2016) Effects of erythropoietin combined with tissue plasminogen activator on the rats following cerebral ischemia and reperfusion. Brain Circulation 2(1): 54–60. https://doi.org/10.4103/2394-8108.178552 [PubMed] [PMC]
Wang RL, Yang ZH, Huang YY, Hu Y, Wang YL, Yan F, Zheng YM, Han ZP, Fan JF, Tao Z, Zhao HP, Li SJ, Luo YM (2024) Erythropoietin-derived peptide ARA290 mediates brain tissue protection through the β-common receptor in mice with cerebral ischemic stroke. CNS Neuroscience and Therapeutics 30(3): e14676. https://doi.org/10.1111/cns.14676 [PubMed] [PMC]
Wu YW, Comstock BA, Gonzalez FF, Mayock DE, Goodman AM, Maitre NL, Chang T, Van Meurs KP, Lampland AL, Bendel-Stenzel E, Mathur AM, Wu TW, Riley D, Mietzsch U, Chalak L, Flibotte J, Weitkamp JH, Ahmad KA, Yanowitz TD, Baserga M, Poindexter BB, Rogers EE, Lowe JR, Kuban KCK, O'Shea TM, Wisnowski JL, McKinstry RC, Bluml S, Bonifacio S, Benninger KL, Rao R, Smyser CD, Sokol GM, Merhar S, Schreiber MD, Glass HC, Heagerty PJ, Juul SE; HEAL Consortium (2022). Trial of erythropoietin for hypoxic-ischemic encephalopathy in newborns. New England Journal of Medicine 387(2): 148–159.https://doi.org/10.1056/NEJMoa2119660[PubMed] [PMC]
Yang M, Wang K, Liu B, Shen Y, Liu G (2025) Hypoxic-ischemic encephalopathy: Pathogenesis and promising therapies. Molecular Neurobiology 62(2): 2105–2122. https://doi.org/10.1007/s12035-024-04398-9 [PubMed]
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Korokin MV, Chatsky IV, Maslinikova MR, Kushnir SA, Pokrovsky VM

This work is licensed under a Creative Commons Attribution 4.0 International License.
 Русский
Русский
 English
English

